“Preceptors are responsible for departmental specific orientation and shaping the development of the new graduate in the early weeks and months of their nursing career. Turnover of direct care nurses has increased at an alarming rate since the start of the pandemic and new graduate nurses continue to be in high demand, but the diminishing number of qualified preceptors presents a challenge. Innovative approaches are needed to make way for increasing the pace of hiring and onboarding new graduates. A group orientation approach was identified as an opportunity to re-design orientation for newly licensed registered nurses in an employer-based transition to practice nurse residency programs. Findings from the first cohort suggest that leaders, preceptors, direct care nurses, and new graduate orientees were satisfied with a group orientation model. Preparing novice nurses to enter practice requires organizational commitment and resources. Group orientation may be a useful approach to foster new graduate nurses’ transition to practice and advance the preceptor role.” (McDermott)
Continue readingCategory Archives: Nurse Retention
Emory Authors: Changes in Posttraumatic Growth After a Virtual Contemplative Intervention During the COVID-19 Pandemic:
“Contemplative interventions can substantively improve posttraumatic growth. This may be particularly relevant for coping with COVID pandemic stress among nurses on the frontlines and for healthcare leaders seeking to strengthen psychological support within their teams and reform the workplace environment”

JONA Highlights: The Effect of Work Stressors on RN Exhaustion
“The conservation of resources theory suggests that individuals experience stress when they are threatened by resource depletion, lost resources, or failure to get resources after a significant effort. When workers continuously face such conditions, they are more likely to experience psychological burnout.”
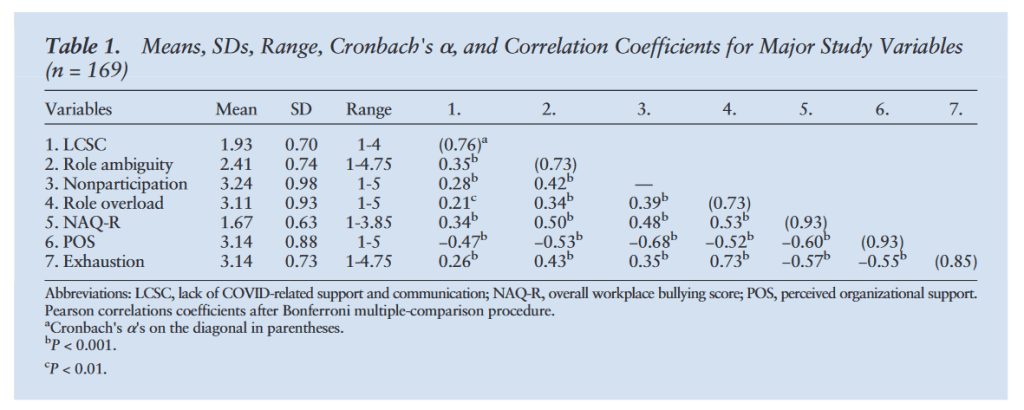
“Stressful and poorly organized work environments may give rise to conditions resulting in bullying. Workplace bullying is the persistent exposure to negative acts, which may be psychological,verbal, or physical. Several work stressors (eg, workload, role ambiguity, decision authority, interpersonal conflicts, tyrannical and laissez-faire leadership behaviors) were associated with bullying.”
Filipova, Anna. (2023). The Effect of Work Stressors on RN Exhaustion: The Role of Perceived Organizational Support. The Journal of Nursing Administration, 53, 146-153.
JONA Highlights: Retention Outcomes of New Graduate Nurse Residency Programs
“Nurse Residency Programs can increase 1-year retention of new graduate nurses. More controlled and comparative studies are needed to evaluate program differences. Nurse leaders need evidence to ascertain which programs are the most effective in supporting retention and return on investment.
Continue readingJONA Update: Recognizing What Meaningful Recognition Is to Nursesas a Strategy for Nurse Leaders
Meaningful recognition to nurses is as diverse as the nursing population. It is important that instruments be developed to capture the rich cultural and ethnic differences in relation to what is considered meaningful recognition to the nursing workforce. Although pay, public recognition, and opportunities for advancement were seen in this study as important forms of meaningful recognition, a deeper exploration across ethnic, racial, and gender groups is needed. This study underscored that one size of meaningful recognition does not fit all.
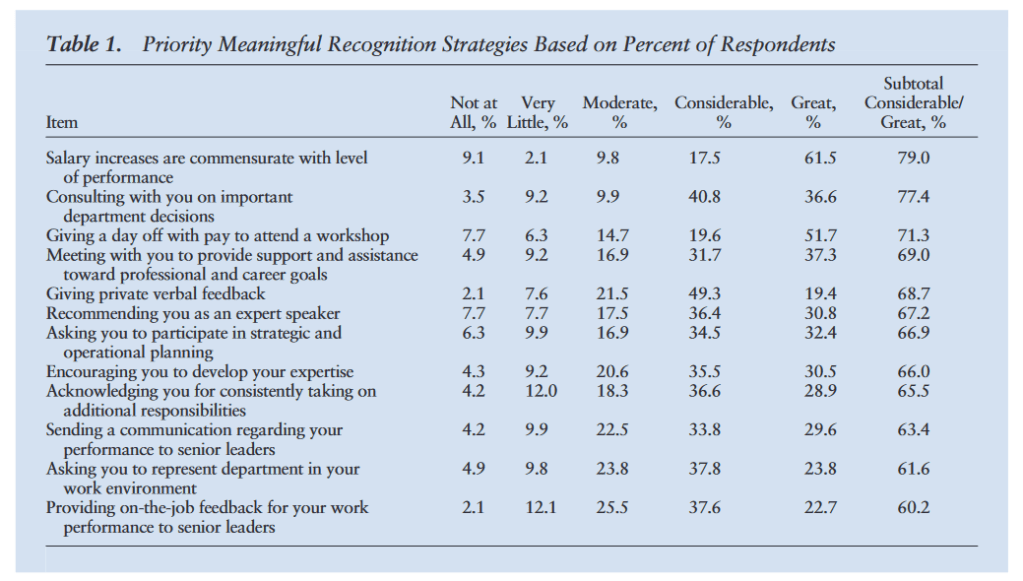
Sweeney, Cynthia, et al (2023). Retaining the Best: Recognizing What Meaningful Recognition Is to Nurses as a Strategy for Nurse Leaders. The Journal of Nursing Administration, 53, 81-87.
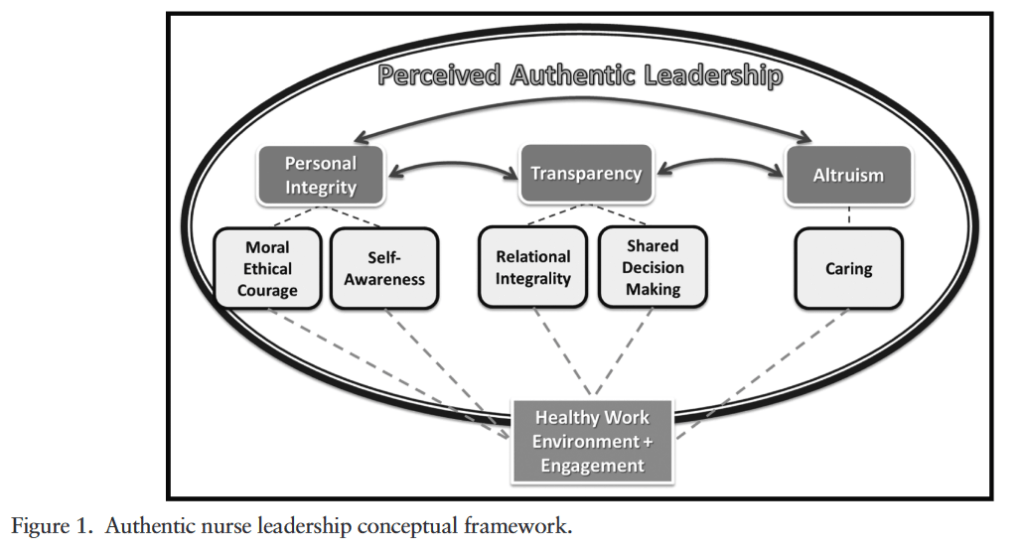
JONA Highlight: Perceptions of Authentic Nurse Leader Attributes Among Clinical Nurses and Nurse Leaders
“This study aimed to develop and validate a tool to measure authentic nurse leadership (ANL) from the perspective of nurse leaders.” (Giordano-Mulligan)
JONA Highlights: Digital strategies to support nursing workflow
The Use of Technology
“Now more than ever, health systems must protect nurses from spending time on work that falls outside of core nursing responsibilities.9 Technology can make life easier for medical professionals and patients alike. It can help relieve the burden on the clinical nurse by enabling some responsibilities to be automated and more expedient, freeing time for nurses to prioritize more critical patient needs. There are numerous innovative technologies leaders should consider integrating into nurse workflow so care teams can think and work in new ways. Examples include the following:
- Technology-driven pumps and monitors that automate the collection of information needed for care
- Smart devices, including automated beds and vital sign monitoring
- Wearables that provide clinical data to the provider
- Virtual rounding technology that prompts patients and family members with questions via text to scale rounding efforts and prioritize needs
- Electronic white boards integrated with the electronic health record to keep patients and families up to date
- Centralized data command centers that integrate multiple systems into a single monitoring center, including coordination of care, requests for services, and discharge tracking
- Robotics to save nursing and ancillary care time 10
- Artificial intelligence to assist with wound assessment and sepsis capture for nurses that results in quality outcomes at lower cost 11
- Tele-technology that enables virtual inpatient care models, including virtual sitter and virtual expert RN models 12
- Mobile apps that enable bidirectional communication between patients and clinicians across all levels of care. These can improve nurses’ access to patient information, streamline communication and patient education, and provide patients themselves more control over their health. When digital health apps have the look and feel of other mobile apps such as Doordash or Netflix, which are already familiar to consumers, they will require minimal or no instruction.”
