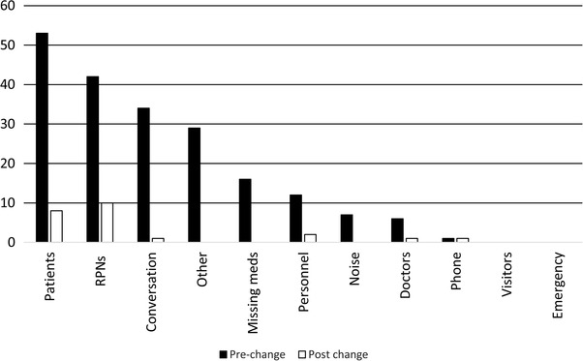
A QI initiative aimed at reducing the number of interruptions and distractions experienced by nurses during the medication administration process examined the effects of:
- introduction of a medication administration room
- standardization of the medication administration process
These changes in practice had significant impact, resulting in “an 88.5% reduction in distractions and interruptions.[1]”
Kavanagh A, Donnelly J. A Lean Approach to Improve Medication Administration Safety by Reducing Distractions and Interruptions. J Nurs Care Qual. 2020 Oct/Dec;35(4):E58-E62. doi: 10.1097/NCQ.0000000000000473. PMID: 32079961.
Full text access for Emory Users.