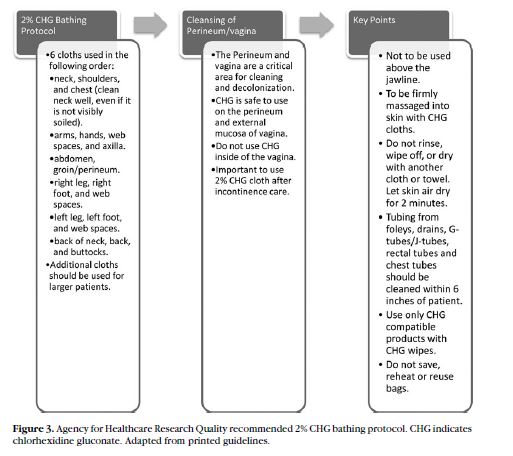
Shah, H. N.,et al. (2016). Bathing With 2% Chlorhexidine Gluconate. Critical Care Nursing Quarterly, 39(1), 42–50
Full Text for Emory Users


Shah, H. N.,et al. (2016). Bathing With 2% Chlorhexidine Gluconate. Critical Care Nursing Quarterly, 39(1), 42–50
Full Text for Emory Users
“Today’s CNS scope of responsibilities encompasses micro, meso, and macro systems levels, and the impact is great. Role responsibilities vary widely, and positioning on the organization chart varies widely as well; CNSs are rising to the occasion. Although a strength of the CNS role can be the variability in the role responsibilities among healthcare settings, it has resulted in challenges in the delivery of education to best prepare for this vital advanced practice role.” (Coke)
Coke, L. A. (2021). Now is the Time for the Clinical Nurse Specialist: Recognizing Value and Advancing the CNS Role. Clinical Nurse Specialist: The Journal for Advanced Nursing Practice, 35(4), 218–219 Full Text for Emory Users
Continue reading“Nursing leaders responsible for orientation are challenged by the plethora of nursing knowledge and clinical skills required by nurses to provide safe care to critically ill patients. The goal is for new and experienced nurses to master the complexities of care and advanced technology and support the well-being of all. One way to achieve this goal is to actively engage new-to-practice nurses and experienced nurses in orientation programs designed to
transfer knowledge and skills needed to provide bedside care”.(Monforto)
Monforto, K., et al (2020801). Outcome-Focused Critical Care Orientation Program: From Unit Based to Centralized. Critical Care Nurse., 40(4), 54-64. Full Text for Emory Users
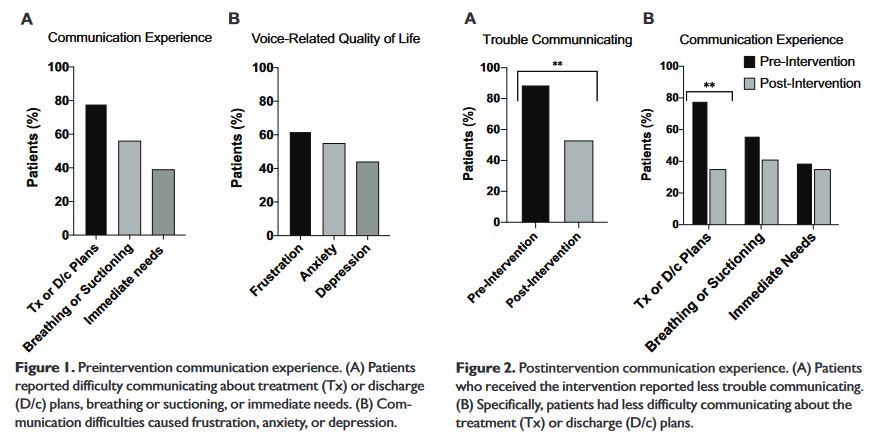
Continue reading“Surgical procedures that render patients acutely aphonic can cause them to experience significant anxiety and distress. Participants in this study included hospitalized patients who
acutely lost the ability to speak due to tracheostomy or total laryngectomy. Acute loss of phonation arising from surgery can be highly distressing for patients, and use of augmentative technology may alleviate some of these challenges by improving communication.”
Haring, C., Farlow, J., Leginza, M., Vance, K., Blakely, A., Lyden, T., . . . Casper, K. (2021). Effect of Augmentative Technology on Communication and Quality of Life After Tracheostomy or Total Laryngectomy. Otolaryngology–head and Neck Surgery., 019459982110137.
Full Text for Emory Users
Arsenic is a carcinogenic environmental factor found in food and drinking water around the world. The mechanisms in which arsenic alters homeostasis are not fully understood. Over the past few decades, light has been shed on varying mechanisms in which arsenic induces cancer. Such mechanisms include gut microbe perturbations, genotoxic effects, and pigenetic modification. Increase in inflammation is the major factor in cirrhosis leading to hepatocellular carcinoma.
Choiniere, J., & Wang, L. (2016). Exposure to inorganic arsenic can lead to gut microbe perturbations and hepatocellular carcinoma. Acta pharmaceutica Sinica. B, 6(5), 426–429.

Continue reading
“Due to the infrequent use of I.V. immune globulin (IVIG) in the oncology population, most nurses have little experience with IVIG administration. Multiple-step calculations are often required to administer IVIG based on patient weight. The cost of a single dose of IVIG can be very high, depending on the formulation. Consequently, administering IVIG can be stressful for nurses. This project has important patient safety implications. It highlights apprehension and distress surrounding IVIG administration and can be used as a guide to identify other areas of opportunity to improve nurse comfort and confidence with high adverse reaction profile medications.”

Barnum, T., Bohnenkamp, C., & Haas, S. (2017). A nursing protocol for safe IVIG administration. Nursing.,47(8), 15-19.
Full Text for Emory Users
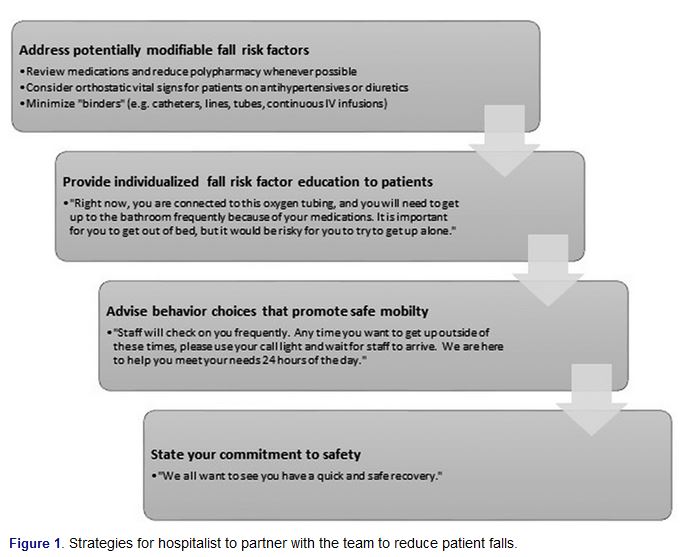
“Despite decades of fall prevention efforts, patient falls remain a common cause of harm in hospitalized older adults. While fall prevention strategies have been historically championed by nurses, hospitalist physicians, nurse practitioners, and physician assistants play a vital role in the multidisciplinary care team in ensuring the safety of our patients. Promising strategies for fall prevention include tailoring interventions to patient risk factors and individualized patient education. In addition to nursing-based interventions, the hospitalist’s role in fall prevention is to (1) identify and address potentially modifiable risk factors, (2) reinforce individualized education to patients, and (3) advise behavior choices that promote safe mobility.”
Keuseman, R., & Miller, D. (2020). A hospitalist’s role in preventing patient falls. Hospital Practice : Advances in Medicine for Primary Care Physicians.,48(Sup1), 63-67.
Full Text for Emory Users