“Employee turnover is a key metric and performance indicator when evaluating the fiscal and operational effectiveness of any health-care facility. This article outlines a turnover analysis and onboarding program performance improvement initiative used by a 187-bed community hospital in the Washington DC metropolitan area to reduce staff turnover. Using an evidence-based approach, we evaluated facility staffing statistics, exit survey data, research literature, and industry exemplars.”
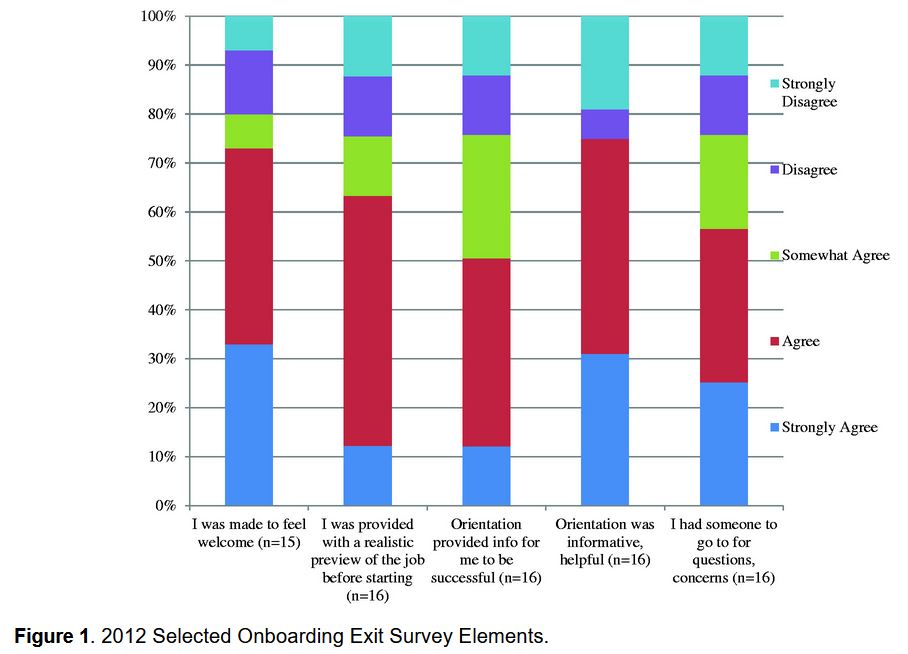
“Exit survey data identified only 50% to 62% of new employees who felt that: hospital orientation provided necessary information for successful employment; they had people to go to with concerns; and they had a realistic understanding of their job.” (Kiel)
Kiel, J. M. (2020). An analysis of restructuring orientation to enhance nurse retention. The health care manager, 39(4), 162-167.
Continue reading