“A significant stressor among nurse managers is the challenge of matching adequate staffing to patient care needs while conserving expenses. Although staffing has been a long-standing challenge, it has steadily grown in complexity since the COVID-19 pandemic. During this time, the number of experienced baby boomer nurses have decreased due to
retirements as younger Generation Z (Gen Z) nurses began entering the profession, creating an “experience-complexity gap.” Meeting the developmental needs of the nursing workforce is just one part of the equation. Gen Z nurses’ changing values toward work
are reflected in their reluctance to work full-time and off-shifts. The increase in part-time nurses means higher numbers of nurses are reporting to individual nurse managers. Further complicating nurse staffing are newer models of care delivery that add licensed practical nurses and virtual nurses into the mix, resulting in increased stress and burnout among
nurse managers. It is imperative that nurse managers implement strategies to mitigate the burdens of their unit workforce.”
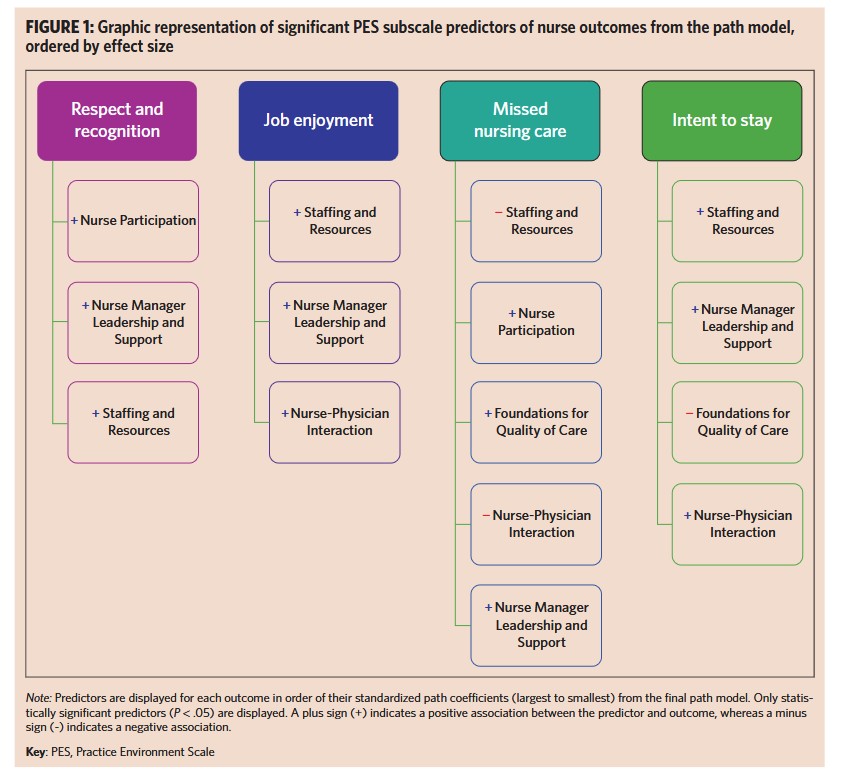
“Based on our analysis, the primary drivers of nurse outcomes were staffing and resource adequacy and nurse manager leadership and support. Nurse-physician interaction and nurse participation in hospital affairs were secondary drivers of nurse outcomes. Interestingly, foundations for quality of care demonstrated unexpected significance; thus, it’s also of importance as a driver. Therefore, to enhance nursing and patient outcomes, nurse managers need to engage in strategies that maximizes each subscale, given the subscale’s
impact on health care delivery”
Losty, L. S., Pascale, A., & Warshawsky, N. E. (2026). Staffing and leadership as drivers of nurse retention: A work environment analysis. Nursing Management, 57(2), 19–26.
